CASE REPORT
Long-term efficacy of omalizumab in patients with conventional treatment-resistant vernal keratoconjunctivitis
Luis Santamaría,1 Jorge Sánchez1,2
1Universidad de Antioquia, Grupo de Alergología Clínica y Experimental, Medellín, Colombia
2Fundación para el Desarrollo de las Ciencias Médicas y Biológicas, Cartagena de Indias, Colombiaa
ORCID
Luis Santamaría, 0000-0001-8709-7383; Jorge Sánchez; 0000-0001-6341-783X
How to cite this article: Santamaría L, Sánchez J. Efficacy of long term treatment with omalizumab in a patient with refractory vernal keratoconjunctivitis. Rev Alerg Mex. 2018;65(2)
Abstract
Background: In vernal keratoconjunctivitis, traditional treatments are sometimes insufficient for symptom control; the results with omalizumab are promising in resistant cases.
Case report: 15-year-old female adolescent with vernal keratoconjunctivitis who had received multiple ophthalmic treatments, immunotherapy and systemic steroids with no clinical response. She attended a clinical immunology and allergy department where she was started on omalizumab 225 mg every 2 weeks. After 6 months, she showed a decrease in pruritus and photophobia; two years later, both papillae and Horner-Trantas dots had disappeared. She remained symptom-free, and the use of ophthalmic drugs was therefore reduced. The patient missed omalizumab application on 4 occasions; however, symptoms recurred, and the papillae reappeared, but remitted upon drug re-initiation.
Conclusion: There is a temporal relationship between omalizumab administration and ocular symptom control, with evidence of relapse upon discontinuation.
Key words: Allergy; Atopy; Conjunctivitis; Vernal keratoconjunctivitis; Omalizumab
Background
Vernal keratoconjunctivitis is a multifactorial disease with chronic inflammation of the ocular surface and may lead to visual loss. Traditional ocular treatments sometimes are not enough to control symptoms but omalizumab is a promising therapy for refractory patients.
Case report
We report one interesting case about a girl of 15 years-old with eye symptoms since she was five years-old. She had received a lot of ophthalmic treatments (antihistamines, lubricants, cyclosporine, tacrolimus, immunotherapy) and systemic steroids without response for their itching, redness, Trantas dots and papillae. Additionally, she was sensitized to house dust mite (Der f and Der p) and had persistent severe rhinitis controlled with nasal treatment. She visited to ophthalmologist who documented glaucoma associated with cyclosporine and steroids and he decided to send to allergology’s service to start systemic treatment. We started omalizumab 225 mg every two weeks (year 2012). After six months the itching and photophobia disappeared. Twenty four months later the patient reported clinical control, and papillae and Trantas dots also disappeared, so we decided decrease dose to 150 mg every two weeks with good tolerance. She remained symptoms free and could reduce her daily pharmacotherapy. She currently has four years and six months of treatment with omalizumab. During this time the patient stopped omalizumab therapy for personal reasons in four occasions, but her symptoms began to reemerge with recurrence of papillae over the following two months. She does recover clinical control when restart omalizumab in the four times (Figures 1 and 2).

Figure 1. Drugs history. Treatments received by the patient for rhinitis and vernal keratoconjunctivitis during the time of follow-up discriminated by the patient's age. The brackets show the time period in which the drug was received. Note: Cyclosporine was received several times at 10 years of age in short cycles as an acute treatment to control symptoms
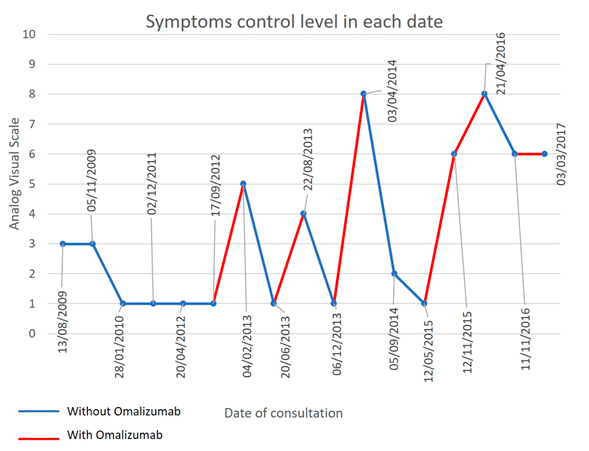
Figure 2. Symptoms control level in each date of consultation. Improvement of the symptoms according patients perception and medical evaluation due to treatment with omalizumab and the clinical deterioration during its suspension is observed
Discussion
Vernal keratoconjunctivitis occurs frequently in the first decade of life and is predominantly in men. Despite including in its name, the term vernal, which refers to its relationship with the summer season and pollination that occurs during that period, patients with vernal keratoconjunctivitis in the tropical regions where there are not seasons have symptoms throughout the year. In addition, patients in those regions are usually not sensitized to pollen grains but sensitization to mites occurs in 80 % of cases.1
In the pathophysiology of vernal keratoconjunctivitis, immediate and delayed hypersensitivity reactions appear to be present, however their exact pathogenesis is still unclear. In contrast to asthma, in which omalizumab may take several months to become fully effective, the onset of action of omalizumab in vernal keratoconjunctivitis seems to be very rapid usually in least than 6 months and total remission of changes in the conjunctiva and/or cornea at 12 to 24 months.2,3 There are less than 10 case reports evaluating the impact of omalizumab in vernal keratoconjunctivitis4,5,6 and the mechanism underlying omalizumab in vernal keratoconjunctivitis, is not clear. In those cases, the patients presented control of ocular inflammatory manifestations and symptoms, as did our patient, however in this report we document a clear relationship between the suspension of omalizumab and the worsening of the symptoms in the patient and the clinical improvement when she restarts it. During the time she received omalizumab, our patient did not present any adverse event, so this treatment seems to be quite safe. Additional studies are required to determine the safety of the use of omalizumab in the treatment of vernal keratoconjunctivitis and to define the appropriate duration of it.
In conclusion, we present a patient with severe vernal keratoconjunctivitis, which was successfully treated with omalizumab with a clear improvement in quality of life, reduction in symptoms and morphologic changes.
References
- López-Piedrahita E, Sánchez-Caraballo JM, Ramírez-Girado RH, Cardona-Villa R. Effectiveness of allergen immunotherapy in patients with vernal keratoconjuctivitis. Rev Alerg Mex. 2013;60(1):11-16.
- Williams PB, Sheppard JD. Omalizumab: a future innovation for treatment of severe ocular allergy? Expert Opin Biol Ther. 2005;5(12):1603-1609. DOI: 10.1517/14712598.5.12.1603
- Sánchez J, Cardona R. Omalizumab. An option in vernal keratoconjunctivitis? Allergol Immunopathol (Madr). 2012;40(5):319-320. DOI: 10.1016/j.aller.2011.08.002
- Doan S, Amat F, Gabison E, Saf S, Cochereau I, Just J. Omalizumab in severe refractory vernal keratoconjunctivitis in children: case series and review of the literature. Ophthalmol Ther. 2017;6(1):195-206. DOI: 10.1007/s40123-016-0074-2
- De Klerk TA, Sharma V, Arkwright PD, Biswas S. Severe vernal keratoconjunctivitis successfully treated with subcutaneous omalizumab. J AAPOS. 2013;17(3):305-306. DOI: 10.1016/j.jaapos.2012.12.153
- Heffler E, Picardi G, Liuzzo MT, Pistorio MP, Crimi N. Omalizumab treatment of vernal keratoconjunctivitis. JAMA Ophthalmol. 2016;134(4):461-463. DOI: 10.1001/jamaophthalmol.2015.5679
Received: 2017-07-05
Accepted: 2018-02-13
DOI: 10.29262/ram.v65i2.292
Correspondence: Jorge Sánchez. jotamsc@yahoo.com
 Todo el contenido de esta revista, excepto dónde está identificado, está bajo una Licencia Creative Commons
Todo el contenido de esta revista, excepto dónde está identificado, está bajo una Licencia Creative Commons
revistaalergia.mx

